It is a common and persistent type of arrhythmia.

Atypical atrial flutter can also be treated with heart ablation and electro-anatomical mapping, although the success rates are not as high.Ītrial fibrillation occurs when there is chaotic electrical activity in the atrium, causing an irregular heartbeat. This may only become evident weeks, months or years after an atrial flutter ablation procedure. Typical atrial flutter can occur alongside both atrial defibrillation and atypical atrial flutter. If you choose a rhythm strategy, a heart ablation procedure may be recommended, as it is generally a favourable alternative to medication. In some cases, a rate versus rhythm strategy may form part of your treatment plan. Your cardiologist may prescribe anticoagulants for this condition in order to decrease the risk of stroke, heart disease, and other conditions. Typical atrial flutter, the most common kind of atrial flutter, occurs in the right atrium. The condition can cause an enlarged left ventricle, which increases the risk of heart failure. Symptoms of atrial flutter vary but often include heart palpitations, shortness of breath, dizziness and fainting. In some cases, the condition can be permanent. This disorganised atrial arrhythmia can lead to malignant arrhythmia, which can be treated with medication, but in some cases, your cardiologist may recommend a heart ablation procedure.Ītrial flutter can be either sporadic (also known as paroxysmal) or persistent and last for days or weeks at a time. Atrial fibrillation that conducts impulses to the ventricles by means of the accessory pathway is known as pre-excited atrial fibrillation. This movement is called antidromic atrioventricular tachycardia. In this case, the electrical impulses move along the bypass tract from the atria to the ventricles and subsequently use the AV node to move from the ventricles to the atria. If electrical impulses move from the atria down the AV node to the ventricles and then use the bypass tract to move from the ventricles to the atria, a particular movement known as the orthodromic-ventricular tachycardia occurs between the atria and ventricles. The condition typically occurs when there is an extra electrical connection (known as an accessory pathway or bypass tract) between the atria and the ventricles. This type of arrhythmia occurs when electrical impulses move in a self-perpetuating and abnormal manner (also known as a circus movement) between the atria and the ventricles. Atrioventricular re-entry tachycardia and Wolf-Parkinson White syndrome.The heart ablation procedure has a success rate of around 95 per cent. In this case, a cardiac electrophysiologist will perform the procedure. This kind of arrhythmia can often be treated with prescription medication, but in some cases, your cardiologist may recommend a heart ablation procedure. This condition occurs when electrical impulses move in a self-perpetuating and abnormal manner (also known as a circus movement) in and around the atrioventricular node. Atrio-ventricular nodal re-entry tachycardia.Supraventricular tachyarrhythmia or atrial arrhythmiascan be categorised into four types. If the tachyarrhythmia originates in the ventricles, it is known as ventricular tachycardia. If the tachyarrhythmia originates in the atria, it is known as a supraventricular.
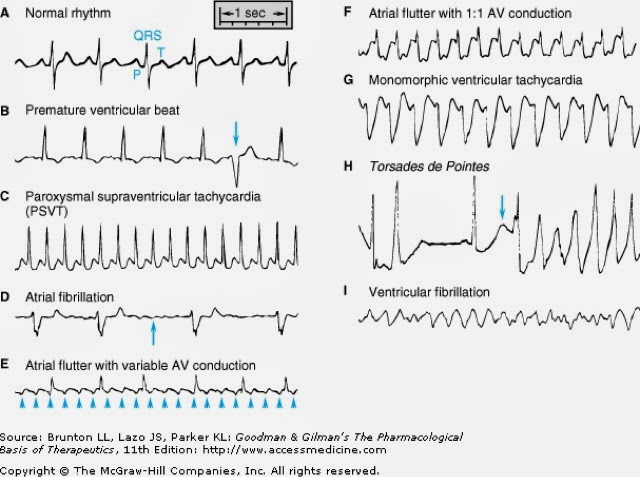
Symptoms of a tachyarrhythmia include heart palpitations, chest pains, shortness of breath, dizziness and fainting. These arrhythmias sometimes occur in normal functioning as well as abnormal hearts.
